Introduction
Prosthetic sockets represent a critical interface between the residual limb and the prosthetic device, where uneven pressure distribution can lead to discomfort, skin breakdown, and long-term tissue damage. Electrical engineers designing sensor systems for medical applications increasingly turn to textile-based sensors to address these challenges. These sensors integrate seamlessly into soft liners or socks, functioning as inner socket sensors to provide real-time pressure mapping without compromising user comfort. Unlike rigid traditional sensors, textile-based pressure sensors leverage flexible fabrics and conductive materials, enabling continuous monitoring during daily activities. This approach aligns with the growing demand for wearable electronics in prosthetics, offering data-driven insights for socket optimization. As prosthetic technology evolves, these sensors bridge the gap between mechanical engineering and biomedical applications.
What Are Textile-Based Pressure Sensors and Why Do They Matter?
Textile-based sensors are flexible electronic components woven or sewn into fabrics, transforming ordinary textiles into responsive pressure detection systems. In prosthetic-socket interfaces, they serve as inner socket sensors, capturing distributed pressure profiles across the residual limb. Pressure sensors of this type detect forces ranging from light contact to high loads experienced during gait, providing spatial resolution that rigid sensors often lack. Their importance stems from the need to mitigate peak pressures that exceed tissue tolerance, which can cause ulcers or neuromas in amputees. By enabling precise pressure mapping, these sensors empower clinicians to refine socket designs iteratively. For electrical engineers, they represent an opportunity to apply circuit design principles to stretchable substrates, ensuring reliable signal acquisition in dynamic environments.
The relevance extends to rehabilitation and long-term prosthesis use, where volume fluctuations in the residual limb alter interface pressures. Traditional measurement tools, often bulky and lab-bound, fail to capture real-world data. Textile-based sensors overcome this by conforming to the limb's contours, maintaining consistent contact. This facilitates remote monitoring, reducing clinic visits and improving patient outcomes. Industry standards like ISO 10328 emphasize structural integrity in lower-limb prostheses, indirectly underscoring the role of sensors in validating load distribution. Ultimately, these sensors enhance prosthetic functionality, making them indispensable for next-generation devices.
Technical Principles of Textile-Based Pressure Sensors
Textile-based pressure sensors operate primarily through capacitive or piezoresistive mechanisms, each suited to the demands of prosthetic interfaces. Capacitive variants rely on changes in capacitance as applied pressure compresses a dielectric layer between conductive electrodes formed by yarns. Conductive threads, such as those with metallic coatings, serve as electrodes, sewn into patterns that create sensor arrays along seam lines. When pressure deforms the textile structure, the gap between electrodes narrows, increasing capacitance proportionally to the force. This principle allows for high sensitivity across large areas, ideal for mapping pressure gradients in sockets.
Piezoresistive textile sensors, conversely, exploit the change in electrical resistance of conductive materials under strain. Pressure alters the cross-sectional area or length of piezoresistive yarns, modulating resistance in a measurable way. Fabrication often involves knitting or embroidering these yarns into fabrics, ensuring stretchability and breathability. Electrical engineers must consider signal conditioning circuits to amplify small resistance variations, accounting for textile hysteresis where recovery lags behind loading. Both types integrate multiplexers for array readout, converting analog signals to digital data via microcontrollers.
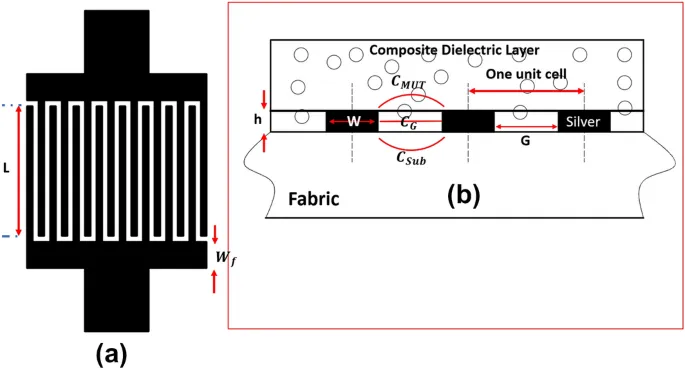
Sensor arrays expand functionality, with grids of 3x3 or larger configurations providing multi-point pressure profiles. Interconnects, also textile-based, route signals to edge connectors interfacing with external electronics. Power efficiency is crucial, as battery-powered wireless modules enable untethered use. Noise from motion artifacts requires filtering algorithms, often implemented in embedded systems. Compliance with IEC 60601-1 ensures electrical safety in medical contexts, guiding isolation and leakage current limits.
Integration and Practical Solutions for Prosthetic Sockets
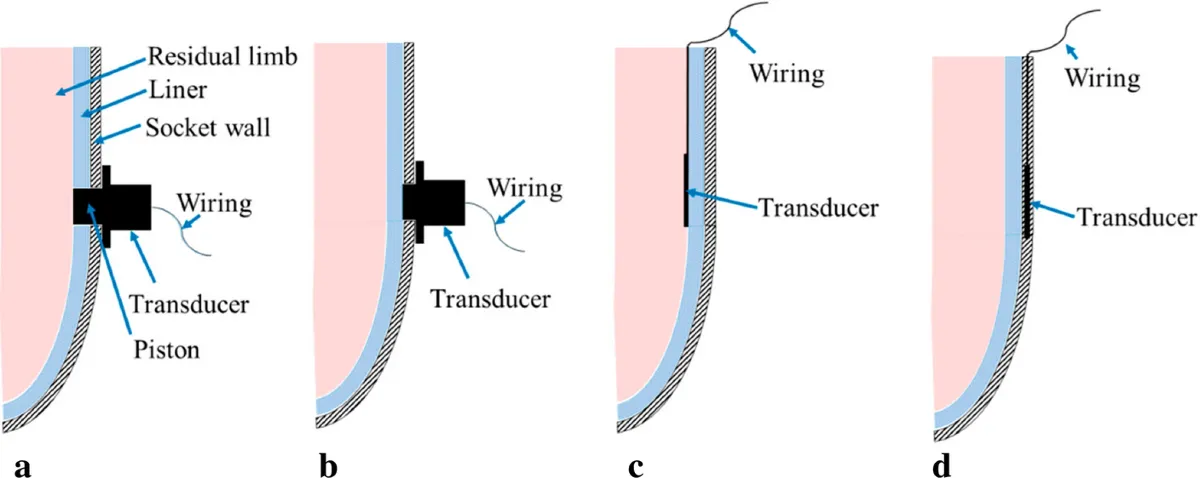
Integrating textile-based sensors as inner socket sensors involves embedding them into liners, socks, or directly into socket walls. A common method uses sewing machines to form seam-line sensors, creating scalable arrays without specialized equipment. These sensors slip between the gel liner and hard socket, capturing interface pressures during stance and swing phases of gait. Data acquisition systems sample at rates sufficient for dynamic events, typically using ADCs with 12-bit resolution for precision.
Calibration remains essential, performed under controlled loads to establish transfer functions. Engineers apply repeatable forces via testing machines, verifying linearity and repeatability. Drift over time, influenced by humidity or sweat, necessitates periodic recalibration protocols. Wireless transmission via Bluetooth Low Energy connects to apps for visualization, alerting users to pressure hotspots exceeding safe thresholds.
Best practices include selecting biocompatible textiles per ISO 10993 guidelines, preventing irritation during prolonged wear. Multi-layer constructions enhance durability, with protective coatings on conductive yarns resisting wash cycles. For array systems, addressing crosstalk between adjacent sensors involves shielding yarns or spatial separation. Engineers optimize readout circuitry for low power, extending battery life in portable units.

Troubleshooting common issues starts with hysteresis characterization, where sensors exhibit path-dependent responses. Advanced designs incorporate elastic dielectrics to minimize this. Shear forces, often coupled with normal pressure, challenge isotropic assumptions; dual-mode sensors measuring both improve accuracy. Finite element modeling predicts stress concentrations, guiding sensor placement at patellar tendon or popliteal region.
Engineering Insights and Emerging Applications
Electrical engineers appreciate the interdisciplinary nature of these systems, combining textile mechanics with analog-digital electronics. Custom PCBs interface sensor buses, handling multiplexing and conditioning before microcontroller processing. Machine learning algorithms analyze gait patterns from pressure data, predicting fit degradation early.
In clinical workflows, sensors validate socket adjustments post-fabrication, correlating peaks with patient feedback. Research demonstrates their utility in pediatric prosthetics, tracking limb growth via pressure shifts. Future iterations may fuse pressure with strain or temperature sensing, creating comprehensive interface monitors.
Conclusion
Textile-based pressure sensors revolutionize prosthetic-socket interfaces by delivering flexible, unobtrusive monitoring as inner socket sensors. Their capacitive and piezoresistive principles enable detailed pressure mapping, informing designs that prioritize comfort and health. Practical integration, guided by standards like ISO 10328 and IEC 60601-1, ensures reliability in real-world use. Electrical engineers play a pivotal role in signal processing and system optimization, advancing wearable biomedical tech. As adoption grows, these sensors promise enhanced prosthetic performance, reducing complications and empowering users.
FAQs
Q1: What are textile-based sensors, and how do they function as pressure sensors in prosthetics?
A1: Textile-based sensors embed conductive yarns into fabrics to detect mechanical deformation. As pressure sensors, they measure interface forces in prosthetic sockets via capacitance or resistance changes. This allows inner socket sensors to map distributions comfortably, aiding fit optimization without rigid components. Their flexibility suits dynamic gait loads.
Q2: Why choose textile-based sensors over traditional rigid pressure sensors for inner socket applications?
A2: Traditional sensors disrupt comfort and breathability in prosthetic sockets. Textile-based sensors conform seamlessly, providing large-area coverage for accurate pressure profiles. They reduce skin irritation risks and enable daily wear, supporting continuous data for clinicians. Electrical integration remains straightforward with low-power electronics.
Q3: What challenges arise in implementing textile-based pressure sensors in prosthetic sockets?
A3: Key issues include hysteresis, drift from environmental factors, and signal crosstalk in arrays. Calibration protocols mitigate these, ensuring repeatability. Biocompatibility and durability under shear enhance reliability. Standards like ISO 10993 guide material selection for safe, long-term use.
Q4: How do inner socket sensors contribute to prosthetic design improvements?
A4: Inner socket sensors deliver real-time pressure data, identifying hotspots during activities. This informs socket modifications, balancing loads per ISO 10328 testing principles. Engineers use the insights for iterative designs, improving tissue health and user satisfaction.
References
ISO 10328:2016 — Structural testing of lower-limb prostheses. ISO, 2016
IEC 60601-1 — Medical electrical equipment - General requirements for basic safety and essential performance. IEC, 2005
ISO 10993-1 — Biological evaluation of medical devices - Part 1: Evaluation and testing within a risk management process. ISO, 2018